This section offers key information about Behavioral Health services for providers. While it is primarily intended for Behavioral Health (BH) providers, medical providers may also find helpful insights to support patients with behavioral health needs. The information listed below is not all-inclusive. Be sure to always check your patient's benefits in Eligibility & Benefits or your practice management system.
The links below will assist you in navigating the behavioral health resources for Blue Cross and Blue Shield of Alabama. Refer to the following categories to learn more:
Logging Into ProviderAccess
Behavioral health providers should have access to and be familiar with our provider website, ProviderAccess. For more information on getting set up, visit How to Register for ProviderAccess.
For your practice’s first visit to the portal, select “Register Now” in the dark blue box on the left.
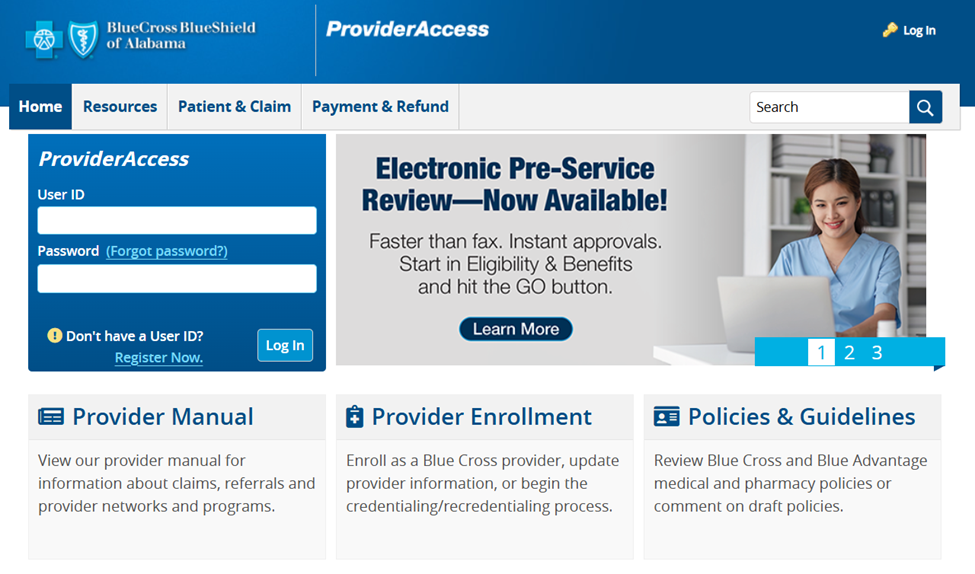
The first user who completes registration for each practice becomes the Master Administrator and will be able to create usernames and passwords for additional staff who need access.
On ProviderAccess, you can:
- Verify patient eligibility and benefits
- Submit claims electronically
- View fee schedules
- Access additional administrative tools
The site also includes a search box in the upper-right corner, which is helpful for quickly locating information.
Back to Top
Behavioral Health Carve-Outs
Some employer groups choose to carve out behavioral health services to another company to manage costs. When this happens, Blue Cross and Blue Shield of Alabama does not process claims for behavioral health services for those patients.
Behavioral health services including mental health and substance use treatments may be covered by a third-party vendor that is separate from the medical plan.
To determine whether behavioral health services are carved out for a specific patient, check Eligibility and Benefits before providing services. Contact the company listed there for claims and service-related questions.
Disclaimer: Blue Cross does not partner with any entity to carve out services based on behavioral health diagnosis (BH Dx). Carve-outs are determined by diagnosis, not by provider specialty.
Back to Top
Blue Choice and Expanded Psychiatric Services (EPS)
Blue Cross offers two primary behavioral health products, each supported by its own provider network: Blue Choice and Expanded Psychiatric Services (EPS). Below is an overview of both programs.
Blue Choice
Blue Choice is a fee-for-service product where patients have a copay for behavioral health services.
Blue Choice providers who need assistance with provider enrollment and contracting, clinical criteria, precertifications, standards of care and related matters should contact Lucet at 1-888-611-6285, Option 3.
For Blue Choice providers who have claims status or remittance questions, first review the information on ProviderAccess, then contact Customer Service. Blue Choice providers can also contact us at 1-866-904-4130.
Expanded Psychiatric Services (EPS)
Expanded Psychiatric Services (EPS) is a managed care product. Providers who need assistance on EPS patients should contact Lucet at 1-888-611-6285, Option 3.
Back to Top
Coding and Documentation
A variety of resources are available to support accurate and compliant clinical documentation. For detailed guidance, refer to the materials located on the Coding and Documentation webpage on ProviderAccess or email CodingConsultant@bcbsal.org.
Back to Top
Direct Deposit/Electronic Funds Transfer (EFT)
To enroll for direct deposit, update your direct deposit account information, or cancel direct deposit, login to ProviderAccess and click Direct Deposit/EFT Registration under Payment & Refund in the main menu.
Note: You must have an active username and password to access the Zelis enrollment hub.
Back to Top
Lucet
Lucet Third-Party Website Disclaimer
By clicking any of the links in the section below, you will be redirected to Lucet’s website. Lucet is our business partner and is an independent company that provides behavioral health services. Lucet has agreed to follow Blue Cross' privacy and security policies regarding the confidentiality and protection of your personal health information.
|
About Lucet
Blue Cross and Blue Shield of Alabama partners with Lucet Health (formerly New Directions) as our Behavioral Health Benefit Manager (BHBM).
Lucet’s Responsibilities
Lucet manages all behavioral health network operations, including:
- Credentialing, contracting, and network management for behavioral health providers, including calculating fee schedules and offering provider education.
- Precertifications and preadmission certifications for behavioral health services.
- Case management and clinical support, including consultation on clinical matters and recommended protocols.
- Provider and, in some cases, member/patient customer service, serving as a central resource for all behavioral health needs.
Lucet Provider Resources
General Resources
Use the Behavioral Health Contacts Guide for quick access to key phone numbers, tools and resources to support behavioral health care for your patients.
Behavioral Health Assistance
To make a case management referral, arrange a call with a psychiatrist, or seek other behavioral health assistance, call Lucet’s physician help line at 1-855-339-1598. This line is available 24/7, including holidays. For general information on Behavioral Health programs, visit Lucet’s website.
Discharge Planning
If you need help with follow-up appointments after discharge for inpatient behavioral health patients, call the Discharge Planner Hotline at 1-800-765-9124. This direct line connects to our Clinical Support Team, which will conduct a screening and schedule a follow-up appointment with the patient.
Provider Portal
Manage patient information, referrals, and access additional support services.
Toolkit
Access practical tools and resources to support behavioral health care delivery.
Contact
Email questions or concerns to providersupport@lucethealth.com.
Back to Top
Medical Policy
Review medical policies regularly to stay informed about updates that may affect service coverage or reimbursement. Several policies may impact behavioral health practices, including those related to transcranial magnetic stimulation, transcranial magnetic stimulation and urine drug testing.
Visit the Medical Policy webpage to view or search Behavioral Health policies.
Back to Top
Out-of-Network Providers
Out-of-Network providers with questions about Behavioral Health should call Customer Service at 1-205-733-7016.
Back to Top
Additional Resources
Major Depression Guideline for Initial Outpatient Treatment of Adults, 2015
Source: American Psychiatric Association and collaboration with Lucet
Importance of Follow-Up After Hospitalization for Mental Illness
Source: National Committee for Quality Assurance (NCQA)
Methadone Treatment - Local Code Deletion
Source: Special Bulletin BS 2002-13
Back to Top
Lucet is an independent company offering behavioral health solutions and services on behalf of Blue Cross and Blue Shield of Alabama.
 FORMS & MANUALS
FORMS & MANUALS
 PATIENT HEALTH
PATIENT HEALTH
 POLICIES & GUIDELINES
POLICIES & GUIDELINES
 PROGRAMS & INITIATIVES
PROGRAMS & INITIATIVES
 Advanced Practice Providers
Advanced Practice Providers